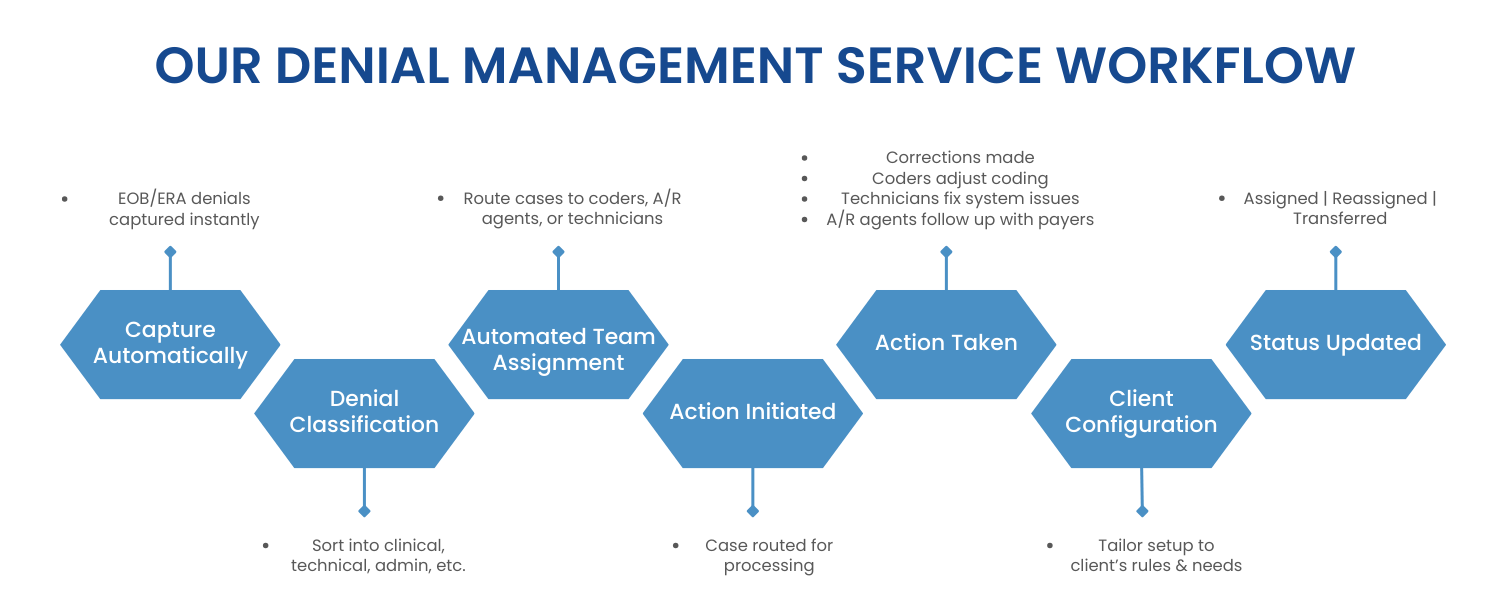
The Results You Get with Our Denial Management Strategies
At RevenueES, our goal isn’t just to manage denials; it’s to deliver measurable improvements to your revenue cycle. By combining denial management solutions, coding denial management services, and comprehensive medical claims denial management, we help healthcare providers see real, lasting results.
Here’s what you can expect when we manage your denials:
- Up to 90% recovery of previously denied claims
- 25–30% higher clean claim rates, reducing resubmissions and delays
- Faster reimbursements that keep your cash flow healthy and predictable
- Fewer repeat denials thanks to root-cause analysis and prevention strategies
- Reduced administrative burden so your staff can focus on patient care, not paperwork
- Improved compliance with payer rules and industry regulations
- Stronger revenue cycle visibility with real-time denial reporting and insights
- Sustainable growth from long-term denial prevention and optimized processes
With RevenueES, every denial turns into an opportunity for recovery, and every claim brings you closer to a stronger bottom line.